Novel Therapeutic Strategies
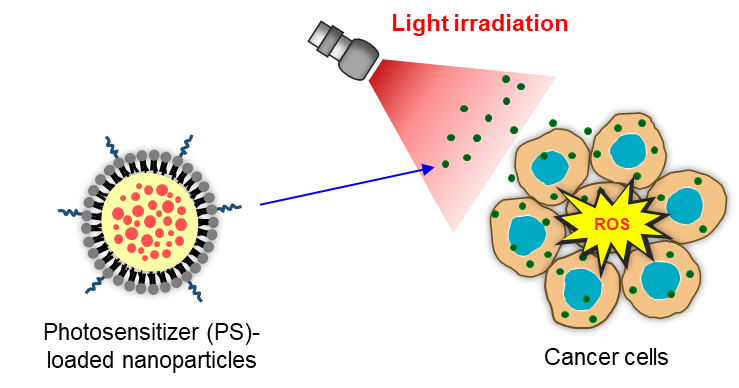
Photodynamic therapy (PDT) has proven to be an effective and minimally invasive modality for cancer treatment, which can be used alone or together with other conventional treatments. PDT requires three harmless key components: photosensitizer, light and oxygen. The treatment protocol is based on the activation of a photosensitizer by using a suitable wavelength of light in the presence of tissue oxygen, which then results in the generation of singlet oxygen or other reactive oxygen species (ROS) to destroy cancer cells. PDT also offers significant benefits to overcome a variety of cancers. Many photosensitizers are hydrophobic and show tendency to aggregate in aqueous solutions, so that encapsulation in drug delivery system may improve their PDT performance.
Recently, our laboratory successfully prepared polymer-lipid hybrid nanoparticles with good biocompatibility to deliver the hydrophobic photosensitizers that expand the therapeutic applications of PDT to multidrug resistant (MDR)lung cancer cells. The formulated nanoparticles have the potential to improve the solubility of photosensitizer. Also, nanoparticles may augment in vitro PDT efficacy by effectively increasing the accumulation of photosensitizer in MDR cells without being affected by the MDR mechanisms, leading to enhanced light-induced generation of singlet oxygen and superoxide anion, which finally causes apoptotic cell death.

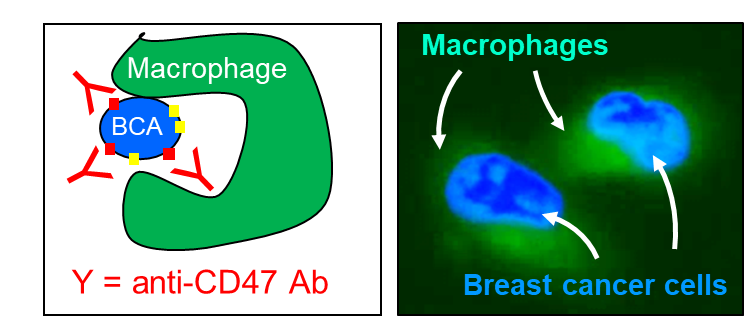
Cancer immunotherapy is another area of interest. Some cancer cells have partner proteins that bind to the checkpoint of native immune cells such as macrophages and cytotoxic T cells, inhibiting their functions. We have explored the potential use of CD47 inhibitors such as anti-CD47 antibody (B6H12) in co-cultures of breast cancer cells and macrophages. Adding anti-CD47 Ab causes macrophages to regain their function and kill breast cancer cells, MDA-MB-231, a triple negative breast cancer cell. We further explored the use of anti-PD-1 antibody in co-cultures of breast cancer cells and cytotoxic T cells. Adding anti-PD-1 Ab can help cytotoxic T cells regain their function and kill MDA-MB-231 cells. In future, we propose to test these blocking effects using cancer cells and blood obtained from patients with breast cancer, which may provide an option of personalized medicine for these patients.